Menopause treatments: your options for symptom relief
While not everyone needs treatment, there are plenty of options available to help you manage menopause symptoms and help improve your quality of life. Here’s what you need to know.

In this article:
- 1/ What is menopause?
- 2/ Menopause hormone therapy and vaginal estrogen
- 3/ Nonhormonal prescription options for menopause symptom relief
- 4/ Self-care and lifestyle strategies
- 5/ Over-the-counter menopause relief and supplements
- 6/ Perimenopause treatment considerations
- 7/ Who should avoid certain therapies
- 8/ How to choose a treatment plan
- 9/ The bottom line on treating menopause symptoms
- 10/ Treating menopause and its symptoms: key takeaways
Deciding on a menopause treatment — which might be best for you and whether you’re even going to treat your symptoms at all — can feel like navigating a minefield. You have tons of questions and it seems like nobody knows the answers. Should you push through and deal with the hot flashes and mood changes without treatment? Is hormone therapy considered safe now or not? What menopause symptoms can even be treated in the first place?
Your healthcare team should be able to answer the above questions (and any other ones you have) and will create a personalized treatment plan based on your symptom type and severity, medical history, preferences, and goals. But it’s important that you’re aware of the benefits and risks of most common types of menopause medication — you’ll be able to speak more openly with your clinician and know what questions you want to ask ahead of time.
This guide will explain what menopause is, what treatments are available, certain safety considerations, and how to choose a treatment plan.

What is menopause?
Menopause is the moment when you’ve gone an entire year without having a menstrual period. On average, this happens around the age of 52. But the term menopause also sometimes describes the entire menopause transition, which occurs in three stages:
1. Perimenopause
Perimenopause is the first stage, and is when your ovaries start to produce varying amounts of estrogen and progesterone. This phase tends to begin in your 40s and can last for up to a decade. Perimenopause symptoms include hot flashes and irregular periods.
2. Menopause
This is less a period of time and more a specific moment. It’s when you have gone one full year without a period and it signals that your ovaries have stopped releasing eggs.
3. Postmenopause
As soon as you’ve hit menopause, you enter postmenopause and will stay in this phase for the rest of your life. While many menopause symptoms improve in postmenopause, some symptoms continue for a number of years. Due to low estrogen levels, you have a higher risk of osteoporosis and heart disease once you reach postmenopause.
No matter which stage you’re in, the aim of treatment for menopause symptoms is to reduce bothersome side effects and support your long-term health. And many forms of menopause treatments can be adjusted over time based on your current symptoms.
How treatment decisions are made
Just as every woman’s menopause experience is unique, every woman’s approach to menopause care should be individualized based on your preferences and your needs. Not everyone will have the same symptoms at the same severity.
Your clinician will dive deep into your health history, current symptoms, treatment goals, and more to come up with the best menopause care plan for you. Over time, menopause symptoms can evolve, so it’s important to share any emotional or physical changes with your clinician and reassess your menopause treatment if needed.
Menopause hormone therapy and vaginal estrogen
Hormone replacement therapy (HRT), also known as menopause hormone therapy (MHT), is by far the most widely known type of menopause medication. It helps supplement the estrogen and progesterone that your body is making in variable amounts or has stopped making. The estrogen is what helps improve menopause symptoms while progesterone is added to help keep your uterine lining from growing too thick. If you no longer have a uterus, you likely will not need progesterone.
There are two main forms of estrogen therapy: systemic therapy (also called whole-body hormone therapy) and vaginal estrogen. Your clinician will be able to help plan the most appropriate menopause treatments for you, but in general:
Systemic therapy may be considered for vasomotor symptoms (VMS) like hot flashes, bone loss, and other common symptoms of menopause.
Local vaginal estrogen may be advised to provide relief for vaginal and urinary menopause symptoms like vaginal dryness.
Systemic hormone therapy
Vasomotor symptoms (VMS) are considered to be the primary symptoms of menopause (it’s estimated that nearly 75% of people going through menopause will have hot flashes and night sweats). Your clinician may recommend you take systemic therapy in some form to help provide menopause relief for these.

Systemic estrogen can be administered via:
Patch
Pill
Ring
Gel
Cream
Spray
Systemic hormone therapy means the estrogen is absorbed into the bloodstream. There, the estrogen circulates throughout the body to help with things like hot flashes. Systemic hormones can have additional benefits too, like protecting bones, and other health benefits that are currently being investigated.
There are some possible health risks to consider with systemic hormones, including a higher risk for breast cancer and blood clots in some people, which is why it’s important to weigh the benefits and risk factors with your clinician.
To minimize your risk, experts recommend taking HRT at the lowest effective dose for the shortest duration possible and using a transdermal route, like a patch, which is likely to be safer than pills.
Vaginal estrogen therapy
Lower dose localized hormone therapy can help target vaginal dryness and discomfort. This therapy comes as a cream, tablet, or ring and the hormones don’t travel around your body. As a result, this form of hormone therapy tends to have fewer risks than systemic hormone therapy.
Nonhormonal prescription options for menopause symptom relief
Not everyone is a candidate for HRT, whether due to personal preferences or health history. People that may be advised against hormonal options may include those with:
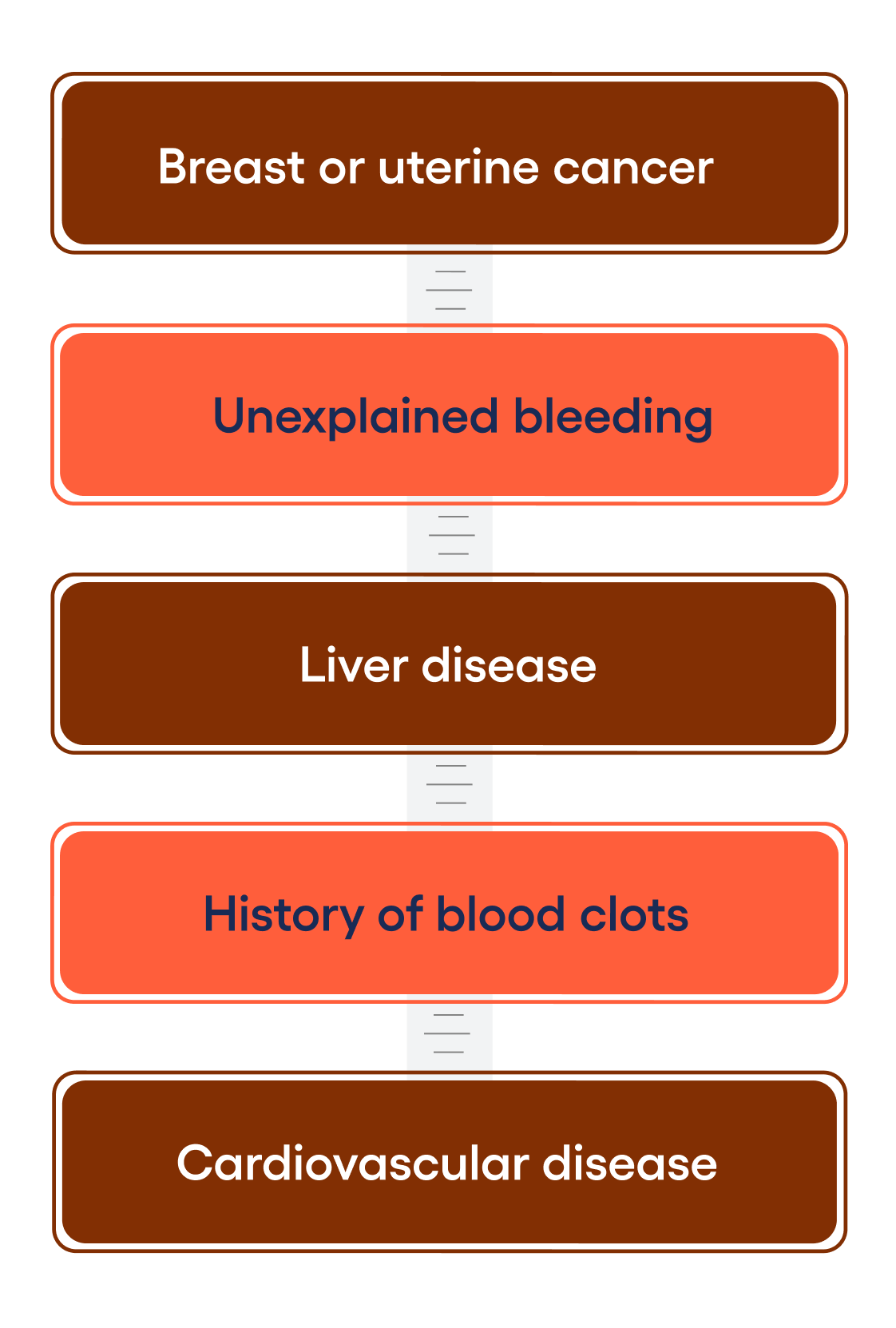
In these cases, your clinician may recommend non-hormonal menopause treatments (or vaginal estrogen if your symptoms are mainly local) to help you feel better. Non-hormonal medications for menopause may include:
Hot flash medications: The FDA has approved some non-hormonal medications specifically to help with hot flashes: Veozah and Lynkuet.
Certain antidepressants: Paroxetine (including Paxil) is a selective serotonin reuptake inhibitor (SSRI) used to treat depression. It’s also a non-hormonal medication approved by the FDA to help relieve hot flashes. And studies also show that other antidepressants, like sertraline, citalopram, fluoxetine, and escitalopram, may offer similar benefits as paroxetine. Some of the most common reported side effects of using SSRIs and SNRIs (serotonin-norepinephrine reuptake inhibitors) include nausea and constipation, which mostly resolves in the first week of treatment.
Seizure medications: Gabapentin (including Neurontin and Gralise) and pregabalin (Lyrica) are antiseizure medications that may help with hot flashes. Potential side effects of both include drowsiness and dizziness. Gabapentin may result in swelling in the arms and legs and Pregabalin may cause weight gain and trouble focusing.
Blood pressure medications: Clonidine (Catapres and others) is approved to reduce blood pressure, but it may also help manage hot flashes. Side effects may include dizziness, fatigue, and constipation.
Bladder antispasmodics: Oxybutynin (Oxytrol) is a pill or treatment option that’s usually used to treat overactive bladders, but it may also help manage hot flashes. Its side effects may include dry mouth and eyes, nausea, constipation, or dizziness.
When considering non-hormonal treatment options for menopause help, be guided by your clinician’s advice on which medication might be best and what dosage to take.
Self-care and lifestyle strategies
Prescription medications are one tool at your disposal, but some menopause symptoms can also be helped with self-care and lifestyle changes. Before making any major changes to your routine or diet, discuss your plans with your healthcare provider.
Diet considerations
While there is limited evidence to support dietary changes improving vasomotor symptoms, there are certain foods that contain phytoestrogens (plant-based compounds with a similar chemical makeup to estrogen). These include soy and flaxseed. While results are mixed, studies have suggested that soy-based isoflavones may help to relieve menopause symptoms. Omega-3 fatty acids are another alternative. They can be found in oily fish, flaxseeds, walnuts, and chia seeds.
Lifestyle factors in managing menopause symptoms
Hot flashes may be reduced by:
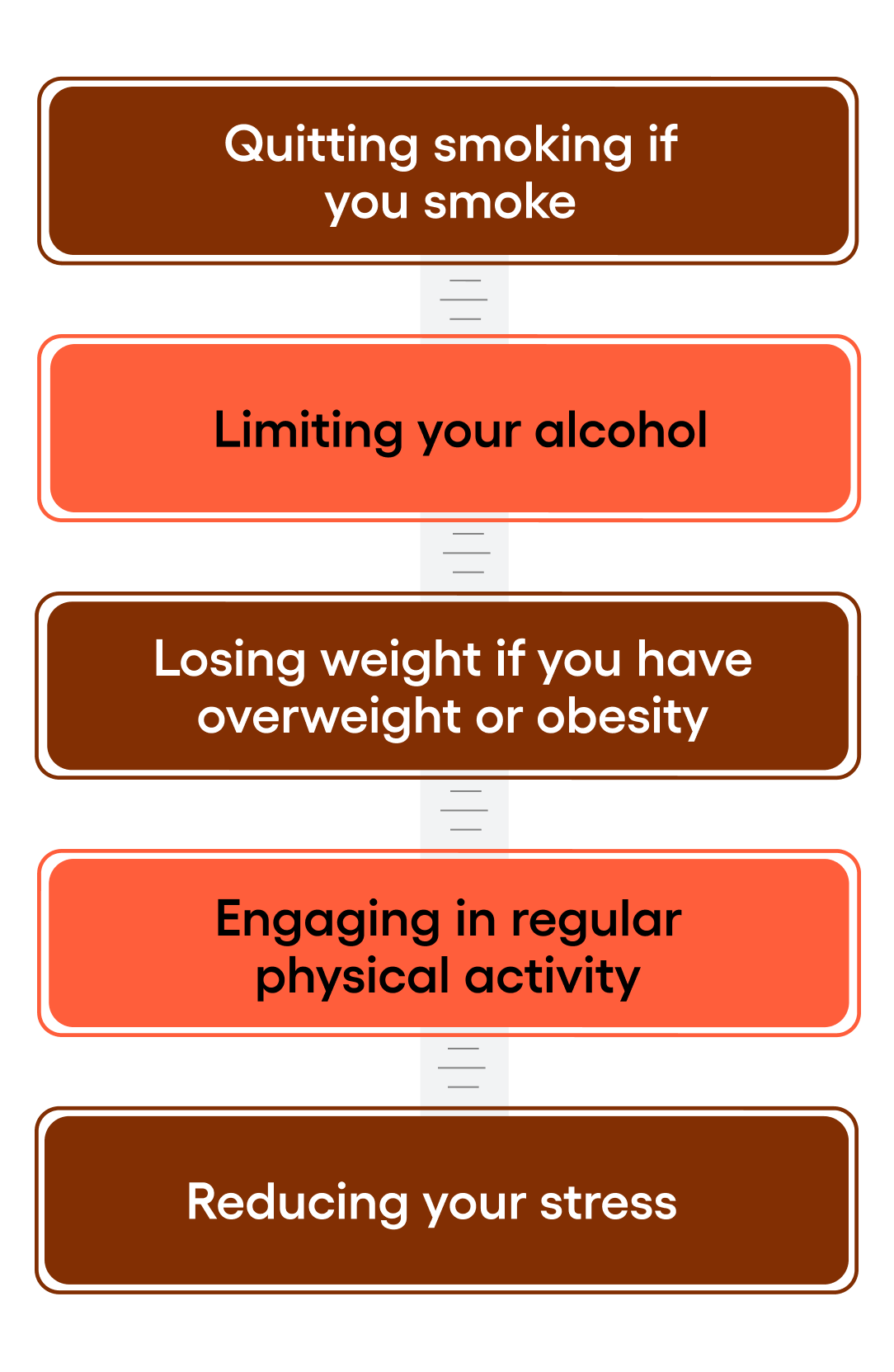
Many of these healthy habits can feel easier to stick with by joining the Weight Watchers Menopause Program. You’ll receive tailored nutritional guidance, join a community of other women going through the same transition, and more. You also have the option to meet with a clinician through Weight Watchers Med+, who can work with you on a personalized treatment plan that may or may not include HRT (if eligible).
Anything that lowers your body temperature can also help, like wearing breathable clothing and turning down the thermostat (especially at nighttime). And if you experience urinary incontinence as a result of menopause, strengthening your pelvic floor with kegel exercises is a good idea.
Over-the-counter menopause relief and supplements
There are some over-the-counter menopause treatments that can help with certain symptoms like vaginal dryness, such as lubricants and moisturizers.
But there are also a lot of supplements claiming to help you improve menopause symptoms, including black cohosh and red clover. It’s a growing industry that’s even been dubbed “menowashing.” But proceed with caution: Supplements aren’t regulated by the FDA, so it’s important to talk to your clinician beforehand to check if it’s suitable for you.
Choosing OTC options wisely
If your clinician gives you the go-ahead, here’s some advice to keep in mind:

Perimenopause treatment considerations
It may feel like your hormones are all over the place during perimenopause — and they are! Hormone changes can trigger symptoms like hot flashes and vaginal dryness. That’s why medications like hormone therapy and vaginal estrogen are often used to treat perimenopause symptoms.
Before choosing any perimenopause treatment, it’s important to discuss your symptoms, needs and personal preferences with your clinician. And remember: If you don’t wish to get pregnant, use birth control throughout perimenopause.
Who should avoid certain menopause therapies and safety considerations
While it can be effective for a lot of people, some individuals may not be suitable to receive certain menopause therapies. This is because systemic hormone therapy may increase the risk of:

If you have strong family history or any of these conditions, discuss with your clinician as you may need to use caution with hormone therapy. Your personal risk of cancer, heart disease, blood clots, strokes, liver disease, and osteoporosis can help your clinician determine whether you may be a suitable candidate for HRT.
Questions to review with your clinician
It’s important to advocate for yourself with your clinician. It may help you to feel more confident asking for menopause help if you have a list of questions to ask.
Use these queries as a starting point for your menopause care and add to them if you have any other specific concerns:
How will I know once I’ve reached menopause?
Are my symptoms caused by menopause or something else?
What menopause treatments may help relieve my particular symptoms?
What lifestyle changes could help me manage my symptoms?
Considering my family and personal history, am I a good candidate for hormone therapy?
How long will my menopause symptoms last for?
How to choose a menopause treatment plan and talk with your clinician
To decide on a menopause treatment plan, you need to discuss your options with a clinician. There are benefits and risks involved with each option and you should weigh them carefully.
To start with, talk about what your symptoms are and which ones are impacting your life the most. This may help you to set priorities as you decide on the right path. Your clinician may suggest a combination of treatments for menopause symptoms, such as HRT and low-dose local products.
It’s easy to lose track, so keeping a symptom log to bring to your appointment may help you feel more informed with your choices. Use your appointment time to ask your clinician any questions you may have as well.
The importance of follow-ups
Your menopause symptoms may evolve over time, so your treatment plan may need to evolve as well. If you notice anything new that worries you, speak to your clinician. You should also pay attention to side effects and report anything unusual to your healthcare provider.
The bottom line on treating menopause symptoms
Menopause can have many different symptoms, and it’s natural to feel unsettled, overwhelmed, and uncomfortable. But luckily, there’s lots of different forms of menopause relief, from hormonal treatments to vaginal creams. The best treatment plan for menopause symptoms is created in partnership with your clinician and personalized to your individual needs and preferences.
Treating menopause and its symptoms: key takeaways
